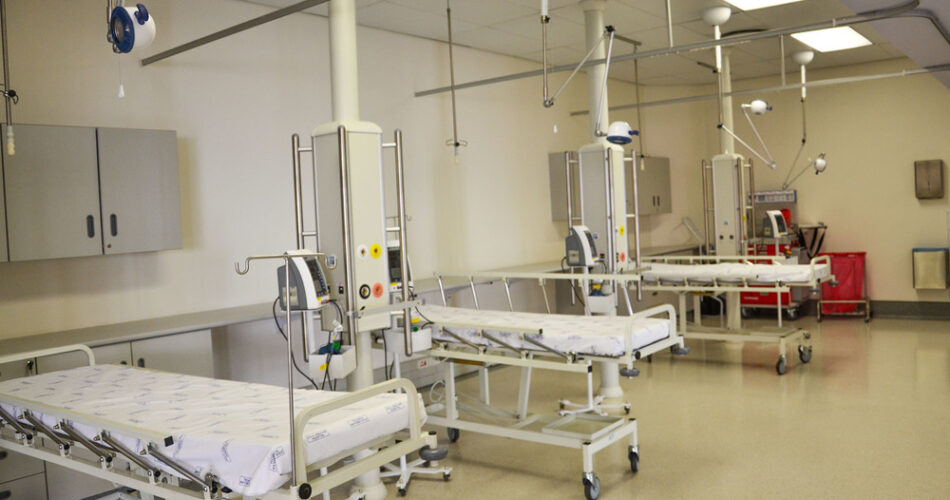
South Africa's medical technology landscape is characterized by deep structural dependencies and systemic inefficiencies. This sector is largely dependent on imports. Photo: supplied
in celebration of World Creativity and Innovation On April 21st, I'd like to begin this piece with an experience many South Africans have: The nurse reaches for a blood pressure cuff that doesn't work. Due to the X-ray machine breaking down, the patient has been asked to come next week. The district hospital had received an imported or donated equipment, which no staff member could maintain, now lying in a store room.
These are not isolated incidents or unfortunate exceptions. Those are recurring patterns — symptoms of a health system that spends billions on technologies it can't effectively use, maintain or replace, most of which are designed and manufactured elsewhere.
Medical technology encompasses any device, apparatus or instruments used to prevent, diagnose, monitor or treat disease – ranging from the most basic, such as a thermometer, bandage or blood pressure cuff, to highly sophisticated devices such as MRI scanners, robotic surgical systems and AI-powered diagnostic platforms. South Africa's medical technology landscape is characterized by deep structural dependencies and systemic inefficiencies. This sector is largely dependent on imports. evaluated according to an estimate R21–29 billion in 2021This sector is almost dependent on imports 90% of its productsGovernment as primary buyer. This dependence is reflected in most low- and middle-income countries (LMICs), where up to 95% of medical equipment is imported and largely financed by international donors.
However, this model provides limited value: the World Health Organization estimates 50-80% medical devicesT is non-functional at any time in under-resourced health systems. More specifically, between 40% and 70% Donated devices remain unused due to poor contextual fit, inadequate planning, inadequate training and lack of maintenance capacity – effectively creating “medical device graveyards”.
In our Innovation Systems research program in the Department of Industrial Engineering at Stellenbosch University, two recent PhD graduates, Dr. Maureen Etucette And Dr. Tinashe Chikunichawahas examined in depth why systems with real technical potential consistently fail to translate that potential into solutions that reach patients at scale. Their work shows that innovators hit the same walls again and again, no matter how good their technology is or how hard they work.
Start at the first wall: Money that comes at the wrong time. The problem is not that South Africa does not fund innovation, but that funding does not follow the journey of a device. As Etucate's 90-stakeholder survey reveals, resource mobilization is both the most important task and the most vulnerable. Funding appears quickly, disappears as risk increases and returns only as risk decreases. The result is predictable: tools stop exactly when they need to go from prototype to validation and scale. The issue is not necessarily the amount of funding, but its structure. Mission-driven pathways are needed that take technologies from initial development to first purchase.
second wall – Regulatory maze – points to a different kind of failure. The rules are not the problem; Shipping capability. Evidence shows how companies reach critical points – certification, export readiness and compliance – and find no clear way forward. Small, local innovators are expected to meet complex requirements without structured guidance, often realizing too late what is required. Government stakeholders regard it as a priority, yet it remains one of the weakest performing sectors. What is needed is not regulation but support: regulatory guidance that helps innovators navigate the system in real time.
third wall – Building the Wrong Thing – is perhaps the most revealing. Tools are missed not because of carelessness, but because the system does not reliably link developers to the actual clinical and procurement needs for the public sector. This is not a design failure, but a system failure. This is reinforced by how technologies reach the market. For most South African health technology enterprises, the path first passes through the private sector – not by choice, but by necessity.
Public procurement is slow, risk-averse and not designed for unproven innovations. Developers are therefore forced to test and refine their products in well-resourced private settings shaped by varying cost structures and patient profiles. The journey is long, and many people do not survive it. They often come out with products calibrated for a completely different system than the one they were originally intended to serve. The implication is clear: demand does not appear quickly. Unless developers are directly connected to the needs of the public sector – from practitioners to procurement – South Africa will continue to produce technologies that work, but not where they are most needed.
fourth wall There is instability of teams. It takes years to create a medical device, but the system rarely lasts long enough for people to perfect it. Intermittent funding and uncertainty repeatedly drive talent away at critical moments. This is not a reflection of personal commitment. This reflects the design of the system.
Amidst all this, the voice of Health Technology Assessment (HTA) is missing. HTA asks questions that the purchase will ultimately demand – does it work, for whom, at what price and compared to what. But for medical devices in South Africa these questions are asked too late. Innovators produce inaccurate evidence, or no evidence at all, and technologies reach procurement without the data needed to drive adoption. The solution is to embed HTA capacity early on – within universities, incubators and innovation programs – so that evidence generation becomes part of the design.
Overall, these insights point to a set of interventions that are less about adding new elements and more about fixing the way existing elements connect. Narrow the demand gap by making clinical need, purchasing criteria and system priorities visible from the start. Embed HTA quickly so innovators can build the evidence the system will need. Create funding pathways that match the lifecycle of a device, not the administrative cycle of a grant. Establish navigable regulatory support so that compliance becomes a process, not a hurdle. And open the way for entry into the public sector – through pilots, conditional procurement and structured testing environments – so that local technologies have the space to prove themselves.
None of them are radicals. All this is already visible, in pieces, within the system. The difference is whether those pieces are connected. What is needed now is the will to invest in innovative infrastructure, because the price of not doing so is paid every day by patients who wait for equipment that does not work and by physicians who cannot treat them because their hands are tied.
Sara Grobbelaar is Professor in the Department of Industrial Engineering at Stellenbosch University.